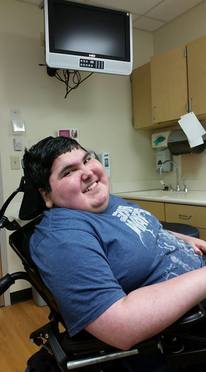
So began a conversation yesterday as Alex and I drove along Interstate I-275 towards Cincinnati Children’s Hospital. The trip capped a stream of hospital visits over the past three weeks. The first included a now-quarterly pulmonary function test (PFT) and visit with Alex’s Pulmonologist. The second included a EEG brain scan to understand his infrequent dizziness and fainting. The third included our now routine Duchenne testing (MRI, EKG, blood work, and x-rays) and follow-up clinic visits with doctors from Neurology, Cardiology, Pulmonary, Endocrinology, Physical Therapy, Rehabilitation, Nutrition, and Social Work. The last visit also included for the first time ever…Palliative Care.
Thankfully, Alex LOVES Children’s Hospital! He loves it not so much for his testing, which can be invasive, long, and sometimes painful (note: his blood draws are notorious for hidden and collapsing veins, which are all too common with Duchenne boys). Alex loves Children’s for the people, even the ones drawing his blood (who he always thanks). He loves the visits for old friends like Herb in lab testing registration or Kenny-Benny in the Duchenne (Cardiac) clinic registration (we call him Kenny-Benny because for years we thought his name was Kenny, when it was actually Benny. Fortunately, Kenny-Benny enjoys the unique name and laughs with us every time). Alex also enjoys visits with nurses, technicians, cafeteria workers, cashiers, janitors, front desk personnel, security guards, and the like. He has come to know many on sight alone. He enjoys meeting new Children’s employees like the friendly technicians and fellows in the EEG testing lab, the Chick-fil-A cow mascot making a special visit yesterday, and anyone riding the elevator with us…to name a few.
Seriously, to name a few. If Alex had more time, he would visit every person on every floor, and then find time to work the parking garage. It’s amazing to watch.
We crossed the Ohio River and headed into Kentucky, towards I-471.
“Who's that?” Alex asked, his curiosity peeked by my revelation of someone new. But this time, he picked up on the emotion we were meeting someone serious. He wondered why I would make a big deal about meeting someone. Don’t they just grow on trees? He knows we have always let him meet people wherever we go. Why prepare him for someone new?
“Well, I’m not sure who it will be specifically. But, today we will be meeting with someone from Palliative Care.”
“Palliative Care? What’s that?” He asked innocently.
The words were understandably foreign to Alex, and to me admittedly when it came to Duchenne. Palliative Care was something in the far future…right? Palliative Care helped patients only in the late stages, correct? However, I knew we had turned a corner and crossed yet another bridge when during our recent visit with Pulmonary the doctor said she was seriously concerned, and wanted to introduce Palliative Care to the team management for Alex. That didn’t sound good.
“Yes. The Duchenne Clinic wants everyone over the age of 18 to begin speaking with Palliative Care,” I generalized, though honestly. For days, I had wondered how to introduce the subject. Alex turning 18 recently seemed the perfect explanation at this stage.
You see, we knew we must prepare him somehow. We knew having Palliative Care walk into our clinic room unannounced would be an odd and difficult pill for Alex to swallow. Best to prepare him beforehand, right? When we were driving to Children’s the morning of his appointments, the timing felt right.
“What do they want to talk about?”
I sighed, feigned distraction from cars driving around us on I-275, and then reached deep within to answer him honestly. Here goes.
“Palliative Care helps older Duchenne boys with quality of life issues. They want to make sure you are living as comfortably as possible and know what you want when things get tough.”
“Comfortable as possible? Know what I want? When things get tough? What do you mean?”
Oh Lord.
As I considered my response, spinning through my head was the prior conversation with Alex’s Pulmonologist about Alex’s declining lung strength since 2009. Over the 8-year span, his pulmonary function has declined LINEARLLY every visit to its meager function today. The trend was not good, and nothing to date helped change its direction. Unless corrected, the trend pointed to trouble ahead. This had not been the first time pulmonary voiced concern. But, it was the first time they have sought Palliative Care to assist.
As I drove through Kentucky and towards the Ohio River, I saw the downward-trending graph in my head. I considered whether to share the words the Palliative Care team uses in their Conversation Starter Kit hand-out. Words like wishes or preferences or worst of all…end-of-life.
Inhale. Exhale. Not now.
Traffic flowed steadily as we crossed over the Ohio River, towards Children’s Hospital, and to our last day of appointments. While driving, I felt the surrealism of Duchenne. I wanted to scream No, we can’t be THERE yet! I wanted to yell this cannot be happening NOW. I wanted to curse Duchenne, repeatedly, and then some more. Instead, I collected my strength, breathed deep, and stay focused on the road ahead.
“Well, at your age, some young men with Duchenne can really have a tough time. They can struggle to understand what’s happening to them. They can worry about their future.”
“What are you saying?” The concern raised in Alex’s voice. I clearly was not explaining as I had hoped.
“I’m saying that, as you know, Duchenne is a hard disease. For some kids, it can get really tough, Some may be overwhelmed with it all…”
Alex abruptly declares his state of mind, of which we are eternally grateful for his resiliency and positive outlook on life.
“Well, that’s not me!” He smiled when I glanced back with relief.
This is truth, and I cannot help join in his smile. His perspective of life…his Duchenne life, in particular…is absolutely beautiful (and the reason I started blogging his journey). Alex sees himself as no different from anyone else, only that he sits down more than others. Despite his physical weakness, he sees himself as an example of happiness and a spreader of cheer. He sees himself as someone who can pick others up just by talking, smiling, and helping them to smile along with him. He shares an interest with everyone he speaks, and with everyone he meets.
Literally.
If you have met Alex, you know what I mean.
But still, the Palliative Care team is not just a formality. They serve a purpose. An important purpose. So much so, Alex’s Pulmonologist wants them on the team, and we agree. I think, subconsciously, Alex understands this, but not fully. He feels his breathing difficulties. He hears the doctors voice their concern. He saw the doctor’s reaction when he asked her the following direct question.
“So, does this mean I am going to die at age twenty?”
Note, this has been a common question Alex has asked over the years, but it was the first time he asked a doctor directly. He held strong as he watched her sigh and pause before responding.
The doctors know his future. They know the challenges he faces. They have seen it before. Sometimes they are blunt. Sometimes they are not. The other day, they were less than either for clear reason. But, the Pulmonologist’s knowing glance to me told me what she truly believed. As a parent, you do everything you can to stay strong for your son. You project strength so he can, too. You project understanding, so he can with time. You project love at every turn.
On the pulmonary front, doctors have prescribed a new and improved ventilator for home use, and a portable ventilator (sip ventilation) to attach to his wheelchair for when we venture outside the home. This morning, Children’s Hospital Home Care spent two hours in our home demonstrating and training us on its usage.
On the cardio front, doctors have expressed concern with new scarring on Alex’s heart. This is the first concern ever shared from Cardiology. Although small, the scarring reminds us the heart is a muscle, too, and that Duchenne could care less of the havoc it creates throughout his body.
For these reasons, Palliative Care is welcome on our team. Things are getting real.
But, for now, our utmost and ultimate goal is to keep Alex’s spirits as high as possible. We must help him to keep the smile on his face. We will do everything and whatever we can to maintain this kid’s joy for life. Those who know Alex will understand what we mean.
We continued driving north on Burnett Avenue, and then pulled into the underground parking garage at Children’s Hospital. I dreaded the visit, and wondered if Alex felt the same way. As he rolled out of the minivan, however, all he talked about was seeing Kenny-Benny. I considered broaching Palliative Care again, but saw no reason. Alex knew how to handle adversity. He knew what he wanted. He wanted time to talk with one of his best friends at Children’s Hospital.
Later, I pulled Alex away from Kenny-Benny and guided him to our clinic room where we spent the better part of the day waiting and talking with the endless stream of nurses, technicians, and doctors. It was a familiar day, one we have enjoyed for nearly 15 years now. For years, Duchenne was a distant monster coming closer. For years, life moved along as best hoped. Only now, do the visits seem real…and vital.
“So, Alex, tell us about what you like to do,” Dr. Widener of the Palliative Care team began. “What makes you happy?”
Classic kid shoulder shrug, followed by awkward silence and searching eyes. Alex, then relaxes and fills the void as only he can.
“I don’t know. People, I guess. I really enjoy meeting and talking with people.”
Smiles all around. A difficult subject appears easier to discuss.
“That’s a wonderful trait to have,” Dr. Widener responded with sincere admiration.
And, so began our meeting with Palliative Care. It was introductory of sorts, thank goodness. I’m not sure we’re ready for the hard topics just yet, the ones to come. But, I could feel Dr. Widener delicately searching for clues on how Alex approaches life. I could sense his gentle handling of very personal worries and concerns. I nodded in thanks for his professionalism and Alex’s incredible attitude. This was Alex’s time to speak, and my time to listen.
“I’m a happy kid.” Alex expressed.
“Yes, we clearly see that. We want you to keep smiling, keep talking, and keep doing what you do.”
Kristy and I couldn’t agree more.
 RSS Feed
RSS Feed